A study published yesterday in NEJM looked at the effect of using cross-sex hormones in gender-dysphoric youth on mental health over a two year period. I don’t think this study provides much useful information, and I hope that we will soon have actual RCTs so that we might know whether these interventions improve mental health.
Note: “Cross-sex hormones” and “Gender-affirming hormones” are used interchangeably in the literature. They use the latter, GAH, in this paper. I will use the term “trans girl” to refer to a male that identifies as a girl, and “trans boy” to refer to a female that identifies as a boy. Given the study participants were mostly minors, I won’t use “trans women” or “trans men” when referring to this study, but the terms are basically the same. You will see “transmasculine” and “transfeminine” if you read the study, once again the nomenclature here is variable in the literature.
Let’s briefly look at what they did and then talk about how to interpret the study:
Psychosocial Functioning in Transgender Youth after 2 Years of Hormones
Study type: Prospective Observational Cohort
Population: 315 participants, average age of 16, range of 12-20. 60% trans boys, 33% trans girls, 6% nonbinary.
Outcome measures: They used five outcome measures (listed below) to assess the effect of cross-sex hormone treatment.
Transgender Congruence Scale
Beck Depression Inventory-II
Revised Children’s Manifest Anxiety Scale
Positive Affect
Life Satisfaction
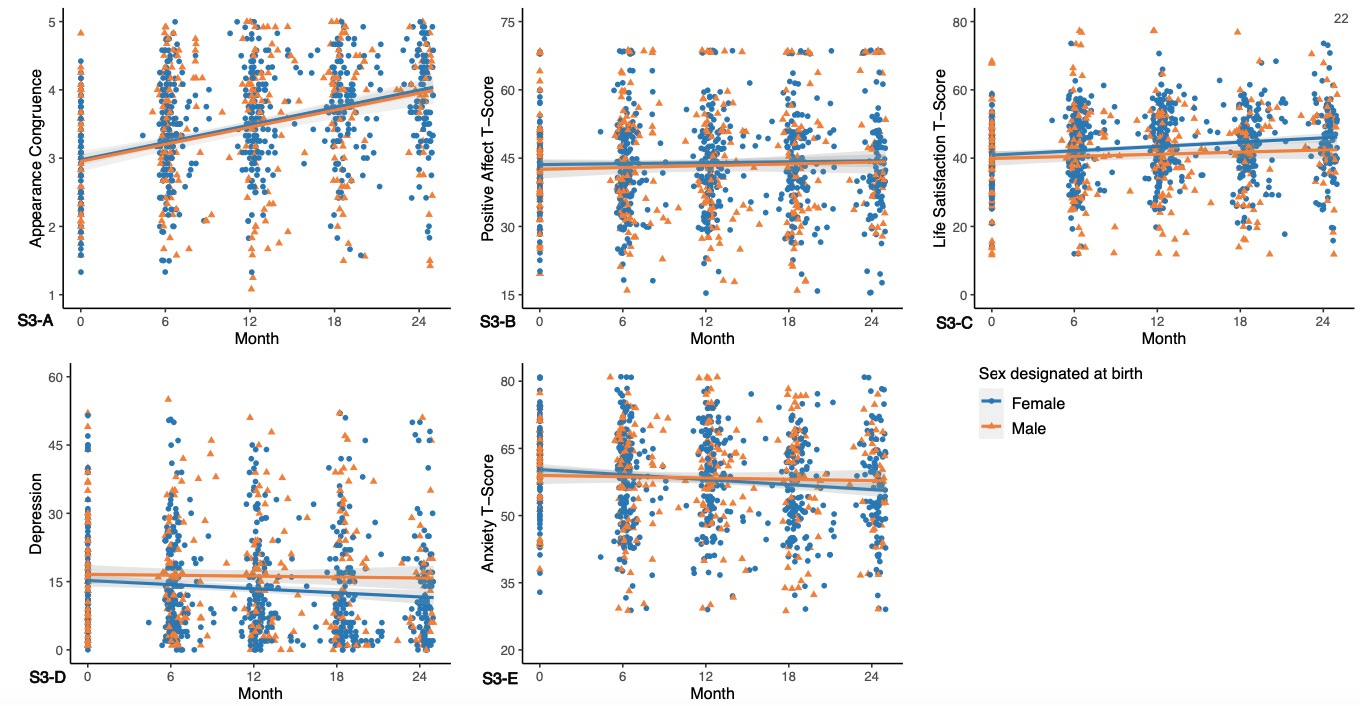
Results: “During the study period, appearance congruence, positive affect, and life satisfaction increased, and depression and anxiety symptoms decreased. Increases in appearance congruence were associated with concurrent increases in positive affect and life satisfaction and decreases in depression and anxiety symptoms. The most common adverse event was suicidal ideation (in 11 participants [3.5%]); death by suicide occurred in 2 participants.”
Interpretation: The most important thing to point out is that this study is unable to tell us whether the use of cross-sex hormones improves mental health. There is no control arm, no placebo, and no randomization. At the end of the day that is the kind of trial required to establish causality. To their credit, the authors briefly mention this in the limitations portion of the discussion, but go on to say, “Overall, our results provide evidence that GAH improved appearance congruence and psychosocial functioning in transgender and nonbinary youth.” Emphasis mine.
This morning the attending physician I was with reminded a room full of trainees of a popular Voltaire quote: “The art of medicine consists of amusing the patient while nature cures the disease.” While this may not readily apply to bacterial endocarditis, it is an important concept to keep in mind in medicine in general, including in patients with depressive and anxious symptoms. Without a control arm we don’t know whether the change in the outcome measures would have happened in the absence of any intervention.
Other observational studies similar to this one have used control arms, but they often are insufficient for a number of reasons. You need randomization at the very least, and placebo controls to have real confidence in the causality of your candidate intervention. Sadly, there are no such studies supporting the use of cross-sex hormones in these populations. We remain in the dark regarding the cost/benefit of this approach.
Let’s temporarily ignore the limitations of this study and just assume that the changes observed are entirely attributable to the hormones. The intervention is radically different for trans boys versus trans girls, who are being given testosterone vs estrogen, respectively. Here we will parse some of the results from above. When the outcomes were noticeably different by intervention, I will mention it below. For each outcome the scale of the test gives some context for the magnitude of change.
Appearance Congruence: This was by far the largest effect seen, and it improved by a full point over the two years on hormones.
Scale range: 1-5
Positive Affect: Did not change from baseline (Statistically insignificant).
Scale range: 0-100
Life Satisfaction: Modest improvement over two years, mostly seen in trans boys. Improved by 4.5 points overall.
Scale range: 0-100
Depression: Small improvement overall (~2.5 points). Improved for trans boys, did not change for trans girls.
Scale range: 0-63
Anxiety: Small improvement overall (~3 points). Once again most improvement was in trans boys.
Scale range 0-100
Final Thoughts: The change in appearance congruence over the two years was substantial. All the other changes far less so. It seems that giving estrogen to trans girls for two years had almost no benefit on depression, anxiety, or life satisfaction. Even if we make an erroneous assumption and attribute causality to the intervention, the actual change in depression and anxiety was minimal. These are serious interventions with lifelong implications, including compromised fertility. To move forward with such interventions in minors with anemic data supporting the practice is rash. We must conduct proper trials to ensure we are not harming minors.
Finally, I should mention another limitation of this study, attrition. In the table below they list the number of participants from which they were able to collect data at each time-point. They were missing roughly 30% of participants in the two year analysis. We are left to wonder why this is and how it might have impacted the results.